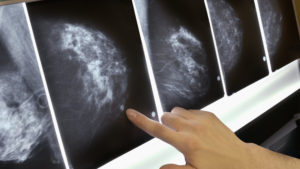
Best Way to Beat Breast Cancer
With rapidly increasing incidence, breast cancer has emerged as a major killer in India with lack of awareness, screening, early detection and appropriate treatment compounding the menace. For the benefit of suffering humanity, Double Helical’s expert panel of specialist doctors from Action Cancer Hospital, New Delhi provides an exclusive insight into the latest procedures and techniques with regard to prevention, screening, diagnosis, and treatment of breast cancer in sync with the international innovations
Breast cancer is a word that generates dread in the minds of women throughout the world. With the rising incidence, this fear has risen exponentially. However, with the growth of modern medicine, the therapeutic armamentarium available to doctors to prevent and treat this disease has too grown simultaneously.
Breast cancer is the fifth most common cause of death due to cancer worldwide. The first four are lung cancer, stomach cancer, liver cancer, and colon cancer. In 2005, breast cancer caused 502,000 deaths (7% of cancer deaths; almost 1% of all deaths) in the world. Breast cancer is the most common cancer among women worldwide.
In India, more and more numbers of patients being diagnosed with breast cancer are found to be in the younger age groups (in their thirties and forties). But 25 years ago, out of every 100 breast cancer patients, 2% were in 20 to 30 years age group, 7% were in 30 to 40 and so on. 69% of the patients were above 50 years of age. Presently, 4% are in 20 to 30 years age group, 16% are in 30 to 40, 28% are in 40 to 50 age group. So, almost 48% patients are below 50. An increasing numbers of patients are in the 25 to 40 years of age, and this definitely is a very disturbing trend. Breast cancer is now the most common cancer in most cities in India, and 2nd most common in the rural areas. Breast cancer accounts for 25% to 32% of all cancers among women in all these cities. This implies, practically, one fourth (or even approaching one thirds) of all female cancer cases pertain to breast cancer.
The overall 5-year survival for breast cancer has increased from 75% in 1970s to almost 89% presently. This means that, out of every 100 women with breast cancer in the US, 89 women are likely to survive for at least 5 years. There are barely any similar statistics for India available, but a rough estimate from the available data is that, this figure is not even more than 60%. The most important reason is lack of awareness about breast cancer and screening of the same; more than 50% patients of breast cancer are reported in stages 3 and 4, so, outcome is not as good as earlier stages despite aggressiveness of the treatment. The western nations have achieved a steadily improving survival rate mainly because of screening of breast cancer.
Breast cancer is a non-existent entity for a majority of population till a near and dear one suffers from it. Healthcare is low on priority and even in major cities, screening is also an ‘alien’ word for most people. So naturally, this results in most people presenting only when symptomatic, and on an average, most ‘symptomatic’cancers reach stage 2B and beyond (significant numbers in stages 3 and 4). So, Indian breast cancer patients do not tend to survive as long as their western counterparts.
In the West, majority of breast cancers (read more than 75%) are reported in stages 1 and 2, resulting in good survival; and there is an ever increasing numbers of patients presenting with mammography detected cancer with no symptoms. India can achieve this goal only with aggressive promotion of screening and awareness and proper treatment.
Cancers in the young, tend to be more aggressive. Many of these cancers are HER2 positive and ER/PR negative, or HER2/ER/PR all three negative, and they have a worse prognosis than those who have ER/PR positive tumours. So, all the more reason to catch these cancers early, since chances of long survival decrease fast with increasing stage of these tumours.
Assessment of all this data shows that with its rapidly increasing incidence, breast cancer is a major public health hazard with multiple physical, social and economic effects and we need to evolve new techniques in the aspects of breast cancer prevention, screening, diagnosis and treatment to counter this threat.
Dynamics of breast cancer management is a very rapidly evolving field. Trials are ongoing throughout the world in the field of breast cancer related to its prevention, screening, diagnosis and treatments. Continuously new techniques are being defined and validated all aimed at improving ultimate patient outcomes in terms of disease control and rehabilitation. The advantage of a more interconnected world is that all the latest innovations in the world in the field of cancers in general and breast cancer in particular are available to us in India.
The ongoing developments and recommendations in the field of breast cancer are outlined below-
BREAST CANCER PREVENTION
Prevention as the term implies aims to prevent the disease from occurring in the first place by removing or reducing the exposure to causative agents. The most important factor in the causation of breast cancer is the exposure of breast tissue to estrogen.The basicparadigm in breast cancer prevention is to lower the exposure of breast tissue to estrogen made by the body.
Decreasing the length of time a woman’s breast tissue is exposed to estrogen helps prevent breast cancer.
Exposure to estrogen is reduced in the following ways:
Early pregnancy: Estrogen levels are lower during pregnancy. Women who have a full-term pregnancy before age 20 have a lower risk of breast cancer than women who have not had children or who give birth to their first child after age 35.
Breast-feeding: Estrogen levels may remain lower while a woman is breast-feeding. Women who breastfed have a lower risk of breast cancer than women who have had children but did not breastfeed.
Estrogen-only hormone therapy after hysterectomy
Hormone therapy with estrogen only may be given to women who have had a hysterectomy. In these women, estrogen-only therapy after menopause may decrease the risk of breast cancer.
Use of chemoprevention (use drugs which reduce the risk of breast cancer) – Selective estrogen receptor modulators
Tamoxifen and raloxifene belong to the family of drugs called selective estrogen receptor modulators (SERMs). SERMs act like estrogen on some tissues in the body, but block the effect of estrogen on other tissues.
Treatment with tamoxifen lowers the risk of estrogen receptor-positive (ER-positive) breast cancer and ductal carcinoma in situ in premenopausal and postmenopausal women at high risk. Treatment with raloxifene also lowers the risk of breast cancer in postmenopausal women. With either drug, the reduced risk lasts for several years or longer after treatment is stopped. Women younger than 50 years who have a high risk of breast cancer may benefit the most from taking tamoxifen. The risk of having these problems decreases after tamoxifen is stopped. Talk with your doctor about the risks and benefits of taking this drug.
In postmenopausal women with osteoporosis (decreased bone density), raloxifene lowers the risk of breast cancer for women who have a high or low risk of breast cancer. Other SERMs are being studied in clinical trials.
Aromatase inhibitors and inactivators
Aromatase inhibitors (anastrozole, letrozole) and inactivators (exemestane) lower the risk of recurrence and of new breast cancers in women who have a history of breast cancer. Aromatase inhibitors also decrease the risk of breast cancer in women with the following conditions:
Postmenopausal women with a personal history of breast cancer.
Women with no personal history of breast cancer who are 60 years and older, have a history of ductal carcinoma in situ with mastectomy, or have a high risk of breast cancer based on the Gail model tool (a tool used to estimate the risk of breast cancer).
In women with an increased risk of breast cancer, taking aromatase inhibitors decreases the amount of estrogen made by the body. Before menopause, estrogen is made by the ovaries and other tissues in a woman’s body, including the brain, fat tissue, and skin. After menopause, the ovaries stop making estrogen, but the other tissues do not. Aromatase inhibitors block the action of an enzyme called aromatase, which is used to make all of the body’s estrogen. Aromatase inactivators stop the enzyme from working.
Risk-reducing surgeries
Some women who have a high risk of breast cancer may choose to have a prophylactic mastectomy (the removal of both breasts when there are no signs of cancer). The ones who are most commonly offered these surgeries are those who are BRCA gene mutation carriers or those with a very strong family history. Such patients can be offered simultaneous breast reconstruction with highly successful cosmetic outcomes. The best and most high profile example of this is Angelina Jolie who chose to have a risk reducing bilateral mastectomy after being diagnosed as being BRCA gene mutation positive. However, it is very important to have a cancer risk assessment and counseling about the different ways to prevent breast cancer before making this decision.
Ovarian ablation
The ovaries make most of the estrogen that is made by the body. Treatments that stop or lower the amount of estrogen made by the ovaries include surgery to remove the ovaries, radiation therapy, or taking certain drugs. This is called ovarian ablation.
Premenopausal women who have a high risk of breast cancer due to certain changes in the BRCA1 and BRCA2 genes may choose to have a risk-reducing oophorectomy (the removal of both ovaries when there are no signs of cancer). This decreases the amount of estrogen made by the body and lowers the risk of breast cancer. Risk-reducing oophorectomy also lowers the risk of breast cancer in normal premenopausal women and in women with an increased risk of breast cancer due to radiation to the chest. However again, it is very important to have a cancer risk assessment and counseling before making this decision. The sudden drop in estrogen levels may cause the symptoms of menopause to begin. These include hot flashes, trouble sleeping, anxiety, and depression. Long-term effects include decreased sex drive, vaginal dryness, and decreased bone density.
Need for exercise
Women who exercise four or more hours a week have a lower risk of breast cancer. The effect of exercise on breast cancer risk may be greatest in premenopausal women who have normal or low body weight.
Screening
Screening is a process to identify the breast cancer cases in the general population before they become symptomatic.
Three tests are used by health care providers to screen for breast cancer:
Mammogram
Mammography is the most common screening test for breast cancer. A mammogram is an x-ray of the breast. This test may find tumors that are too small to feel. A mammogram may also find ductal carcinoma in situ (DCIS). In DCIS, there are abnormal cells in the lining of a breast duct, which may become invasive cancer in some women.
The following may affect whether a mammogram is able to detect (find) breast cancer:
The size of the tumour.
How dense the breast tissue is.
The skill of the radiologist.
The quality of the mammogram machine
Women aged 40 to 74 years who have screening mammograms have a lower chance of dying from breast cancer than women
who do not have screening mammograms.
The field of mammography has been revolutionized by the advent of digital mammography. In digital mammogram thee images can be captured andstored directly onto a computer. However, because digital images are viewed on a computer, they can be lightened or darkened, and certain sections can be enlarged and looked at more closely and results in a much higher sensitivity and specificity. This makes digital mammography better than film mammography for most women especially in women –
Premenopausal or peri-menopausal
Under age 50
Have dense breast tissue
Most leading cancer institutes now have digital mammography machines.
MRI (magnetic resonance imaging) in women with a high risk of breast cancer
MRI is a procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body. This procedure is also called nuclear magnetic resonance imaging (NMRI). MRI does not use any x-rays.
MRI is used as a screening test for women who have one or more of the following:
Certain gene changes, such as in the BRCA1 or BRCA2 genes.
A family history (first degree relative, such as a mother, daughter or sister) with breast cancer.
Certain genetic syndromes, such as Li-Fraumeni or Cowden syndrome.
MRI finds breast cancer more often than mammograms do, but has a slightly lower specificity.
Tissue Diagnosis
Standard methods for acquiring tissue diagnosis for breast cancer have been a FNAC (Fine needle aspiration cytology and a core (needle)biopsy. However, with the advent of advanced radiological techniques which can now detect impalpable asymptomatic lesions these methods fall short. This shortfall has been made up by the advent of image guided core needle biopsy(CNB) and vacuum assisted biopsy (VAB).
Imaging-guided CNB
Due to tissue heterogeneity in breast lesions, the reliability of needle biopsy depends on accurate collection of lesion samples, and the ability of these samples to represent the lesions are critical for the pathologist to make the correct diagnosis. The blind nature of CNB requires multiple biopsies to be performed, and is associated with a certain probability of underestimated and misdiagnosed results. Hence, sampling accuracy is essential for the success of this procedure. Ultrasound- or mammography-guided CNB is now performed for non-palpable breast tumors or breast calcification and achieves much higher accuracy.
Vacuum-assisted biopsy (VAB)
Vacuum-assisted biopsy (VAB) is a new imaging-guided biopsy approach introduced after fine needle aspiration cytology and core needle biopsy (CNB). This technique can completely resect small breast lesions and provide adequate, continuous tissue samples for pathological diagnosis via a single procedure while minimizing injury to breast tissues and maintaining the shape, it has been widely used for the early diagnosis of breast cancer and excision of benign lesions. VAB can be carried out by using the following guidance technologies-
Stereotactic X-ray
This technology is mainly used for non-palpable lesions that are not detectable by ultrasound. Clusters of micro calcifications, structural distortion, small echogenic nodules and radial scars are the common manifestations of such lesions on a plain film. This easy-to-operate approach enables safe and precise positioning, and is particularly sensitive for micro calcifications.
High frequency ultrasound
This non-radioactive, real-time guiding approach is mainly used for the diagnosis of ultrasound-visible BI-RADS 3-5 breast lesions and axillary involvement, which has certain advantages in the patient comfort, operating time, and cost. It has become the most accurate and preferred guidance modality for minimally invasive breast biopsy.
Breast MRI
This is mainly used to display suspicious malignant lesions that are only visible to MRI and undetectable by X-ray, ultrasound or other testing methods. Additionally, it can be used to exclude the presence of malignancy in the case of suspected benign disease based on prior MRI examination (37). Compared with 1T and 1.5T MRI, 3T MRI has a higher sensitivity for breast cancer.
Accuracy of VAB
Suitable for a wide range of applications, VAB is able to obtain sufficient and continuous histological specimens, allowing higher diagnostic accuracy and specificity, and is thus considered to be an ideal alternative to surgical biopsy.
Frozen section
In a proportion of cases of breast lumps, diagnosis cannot be made regarding its nature even after multiple FNAC or biopsies. In such cases of diagnostic dilemmas, the advent of highly accurate frozen section facility at oncological centres has been a boon for patients. A frozen section allows the surgeon to remove the lump and to get the biopsy report within 15 minutes while the patient is still under anesthesia and get a diagnosis. In case of a report confirming cancer, the complete cancer surgery can be performed in the same sitting obviating the need for a second surgery and a delay of around 1 week as was previously required.
STAGING WORK UP
Subsequent to diagnosis, the next step in breast cancer management is adequate staging of the disease so as to guide the treatment plan. The standard staging tests have been a chest x-ray, ultrasound of the abdomen/CECT chest and abdomen and a bone scan. The advent of PET CT now provides us with a single investigative modality with a higher diagnostic sensitivity and specificity. A PET CT scans the whole body for assessing cancer spread and can identify disease at sites which may have been missed with other tests. It is now rapidly gaining acceptance as the standard staging tool for breast cancer.
PET CT
PET/CT is a nuclear medicine technique which combines a positron emission tomography (PET) scanner and an x-ray computed tomography (CT) scanner, to acquire sequential images from both devices in the same session, which are combined into a single superposed (co-registered) image. Thus, functional imaging obtained by PET, which depicts the spatial distribution of metabolic or biochemical activity in the body can be more precisely aligned or correlated with anatomic imaging obtained by CT scanning. Two-and three-dimensional image reconstruction may be rendered as a function of a common software and control system.
PET-CT has revolutionized medical diagnosis in many fields, by adding precision of anatomic localization to functional imaging, which was previously lacking from pure PET imaging. For example, many diagnostic imaging procedures in oncology, surgical planning, radiation therapy and cancer staging have been changing rapidly under the influence of PET-CT availability, and centres have been gradually abandoning conventional PET devices and substituting them by PET-CTs. Although the combined/hybrid device is considerably more expensive, it has the advantage of providing both functions as stand-alone examinations, being, in fact, two devices in one.
The algorithm of management of breast cancer like other cancers follows the basic steps of diagnosis followed by staging work up followed by treatment planning and the actual treatment.
For early breast cancer, the staging work up includes only an x-ray of chest while for advanced breast cancers, a CECT of the chest and abdomen and a bone scan are recommended. Over the past few years, PET CT has emerged as the preferred staging tool for many cancers. In breast cancer too, PET CT is fast emerging as the preferred staging method for advanced breast cancers due to multiple advantages.
SURGICAL MANAGEMENT OF BREAST CANCER
Breast Conservation surgery (BCS)
The field of surgery has rapidly evolved for breast cancer. Prior to the late 19thcentury, breast cancer was regarded as a terminal disease with no treatment options available. In the late 19th century when Halsted carried out the first surgical resections for breast cancer it involved performing a radical mastectomy. This laid down the basis for the surgical treatment of this disease. Halstedian mastectomy while effective was a very mutilating surgery.
Over the years techniques were modified with emphasis on less morbid procedures. This involved the advent of less mutilating modified radical mastectomies. However, it still entailed removal of the entire breast with its attendant physical and psychological costs. Thus trials were begun to evaluate the efficacy of breast conservation techniques. These entailed the removal of the lump along with the axillary lymph nodes thus preserving the remainder of the breast. Multiple trials have shown that BCS is as safe as a conventional mastectomy in terms of overall survival with a lower psychological morbidity.
BCS can now be safely offered to majority of breast cancer patients.
Sentinel node biopsy
The surgery of breast cancer has conventionally involved axillary dissection which entails removal of the axillary lymph nodes which provides both prognostic in formation as well as therapeutic benefit. However, axillary dissection while being the gold standard for axillary staging is associated with significant morbidity in terms of lymphedema, shoulder stiffness and dysfunction. Further, it has been seen that of all patients who undergo axillary dissection only 30% actually harbour disease in the lymph nodes. Hence 70 % patients undergo axillary dissection with its side effects without any therapeutic benefit. Sentinel node biopsy has now emerged as a safe alternative to axillary dissection with a better side effect profile.
Sentinel node biopsy is based on the concept that lymphatic drainage from the breast first drains to a sentinel node and then subsequently drains to the second echelon nodes. Thus identification and removal and assessment of the sentinel node can provide information about the status of the axillary lymph nodes.A surgeon injects a radioactive substance, a blue dye, or both near the tumour to locate the position of the sentinel lymph node. The surgeon then uses a device that detects radioactivity to find the sentinel node or looks for lymph nodes that are stained with the blue dye. Once the sentinel lymph node is located, the surgeon makes a small incision (about 1/2 inch) in the overlying skin and removes the node.
The sentinel node is then checked for the presence of cancer cells by a pathologist.
A negative SLNB result suggests that cancer has not developed the ability to spread to nearby lymph nodes or other organs. A positive SLNB result indicates that cancer is present in the sentinel lymph node and may be present in other nearby lymph nodes and, possibly, other organs. Axillary dissection can thus be restricted to those who actually need it. A sentinel node biopsy has been found to be equivalent to conventional axillary dissection with much lower incidence of side effects like arm swelling (lymphedema), shoulder stiffness and dysfunction.
Breast Reconstruction
Both a mastectomy and a breast conservation surgery lead to both physical and psychological effects on the patient due to loss/ deformity of breast tissue. This aspect can now be tackled with development of new and highly effective breast reconstruction techniques. Microvascular free flaps are now being used for complete breast reconstruction following a mastectomy. These can be performed simultaneously with the primary surgery or a second surgery later on. Microvascular free flaps use the patient’s own tissues which are harvested and transplanted to the chest wall. Free flaps offer nearly perfect aesthetic outcome for the patients and are a boon for breast cancer patients. Free flaps commonly used for breast reconstruction are a free DIEP, free LD, free ALT and a free SIEP flap.
Oncoplastic techniques have also been developed for cosmetically reconstructing the breast after a breast conservation surgery. These involve reshaping and remodeling of the patient’s own tissues for achieving optimum reconstructive outcome.
The development of advanced reconstructive options is a boon for patients of breast cancer who can now no longer need to worry about their body image post-surgery.
Chemoport
A large proportion of patients need chemotherapy as a part of treatment of breast cancer. Chemotherapy involves infusion of the chemo drugs through the veins. Most of these drugsrequire prolonged infusion and are highly toxic and lead to severe thrombophlebitis (painful arm swelling). Further, in breast cancer patients, the arm on the affected side due to cancer is often not available for cannulation due to risk of lymphedema. Thus venous access is often troublesome in breast cancer patients undergoing chemotherapy which becomes a source of considerable anxiety. This can now be overcome by the availability of chemoports for infusion of chronotherapy. A port is a small medical appliance that is installed beneath the skin. A catheter connects the port to a vein. The port is usually inserted in the upper chest (known as a “chest port”), just below the clavicle or collar bone, leaving the patient’s hands free. Under the skin, the port has a septum through which drugs can be injected and blood samples can be drawn many times, usually with much less discomfort for the patient than a more typical “needle stick”. A patient is thus spared the trauma of repeated needle sticks and thrombophlebitis. Availability of chemoports has now reduced the physical and psychological trauma associated with chemotherapy to a large extent.
RADIOTHERAPY
Radiotherapy is part of treatment for a large proportion of breast cancer patients. Radiotherapy uses radiation, such as x-rays, gamma rays, electron beams or protons, to kill cancer cells or damage them so they cannot grow or multiply. It is a localized treatment, which means it generally affects the part of the body where the radiation is targeted. However, most conventional radiotherapy techniques are associated with scatter of the radiotherapy waves to other adjoining body parts which leads to potentially deleterious effects on normal body tissues. In breast cancer, old techniques of radiotherapy were associated with significant toxicity tothe lungs and the heart. These have now been overcome by IGRT.
IGRT/IMRT
IGRT (Image guided radiotherapy) and IMRT (Intensity modulated radiotherapy) are two recently developed techniques of delivering radiotherapy. In these, the radiation planning and delivery is done with the aid of computer simulation which helps in delivering a high dose to the target tissue with minimal scatter and exposure of adjoining body tissues. These techniques have thus greatly reduced the side effects and toxicity associated with radiotherapy while maintaining and enhancing the therapeutic benefit. In breast cancer, application of these two techniques has reduced the cardiovascular(heart) and pulmonary (lung) toxicity.IMRT and IGRT are now fast becoming the standard of care for delivering RT to many organ sites including for breast cancer.
ACCELERATED PARTIAL BREAST IRRADIATION (APBI)
One of the drawbacks of conventional radiotherapy is the prolonged duration of treatment(5 weeks in case of breast cancer) and the need for daily visits to the hospital. This has been associated with logistical issues for many patients and contributed to the reluctance associated with taking radiotherapy even when it is clearly beneficial. This problem can now be addressed with the developing field of APBI (Accelerated partial breast irradiation). In APBI a special machine is used to give a high dose of radiotherapy to the patient in the OT only during surgery. Thus the entire treatment of surgery and radiotherapy is completed in asingle sitting only. This obviates the need for prolonged OPD visits. APBI has been studied in multiple trials and has been found to be effective for patients with early stage breast cancer undergoing breast conservation surgery. APBI is a thing to look out in the future in the field of breast cancer management.
TARGETED THERAPY
The standard systemic therapy for breast cancer has been chemotherapy. While chemotherapy has definitely improved the outcomes in both early and advanced breast cancer, it is also associated with significant short as well as long term morbidity. This is due to the fact that standard chemotherapy drugs are toxic molecules and exert their effect by killing the rapidly dividing cells. Generally the fastest dividing cells are the cancer cells and are the ones most affected by the chemo drugs. However, cells at normal body sites and other body tissues like hair, mucosal linings like mouth and intestines etc are also rapidly dividing and hence get affected by the chemotherapy drugs because of non-specific nature of their action leading to side effects like hair fall, mouth ulcers, diarrhea etc.
Targeted therapies have now been developed to tackle these problems associated with systemic therapies. Basically, the concept of targeted therapy involves the development of molecules that target specific molecules or pathways that are unique to the cancer cells and kill them. These drugs, therefore, selectively target the cancer cells without affecting the other normal body tissues. Therefore, these drugs have much lower side effects than standard chemotherapy. Herceptin (trastuzumab) is the most commonly used targeted therapy in breast cancer and has greatly benefited patients of both early and advanced breast cancer. Other targeted therapy molecules being used in breast cancer are lapatinib, pertuzumab and neratinib. The development of targeted therapies has improved survival while at the same time lowering the side effects of treatment.
ADVENT OF DEDICATED BREAST CANCER UNITS
Of all the developments in healthcare, one of the most impactful feature has been the advent of specialized medicine. Specialized medicine involves the setting up of dedicated units which are designed to tackle specific disease or groups of diseases. In cancer management, this involves setting up of organ specific cancer units. Specialized breast cancer units are the normin leading cancer centres throughout the world and is being rapidly emulated in India. Such units comprise of a team of dedicated professionals including cancer surgeons, medical oncologists, radiation oncologists, pathologists, radiologists, nurses, other paramedical staff and physiotherapists whose sole aim is to provide the holistic care for the breast cancer patient. The results in terms of quality of care like accurate early diagnosis, standardized investigation, work up protocol based word class treatment, post therapy care and patient outcomes like overall patient survival are significantly higher with such dedicated units as compared to treatment in general centres. The development of such specialized teams and units is going to be the norm in the future.
Cancer Patients needn’t live with pain
By Dr G N Goyal
Early detection is the key to the cure of cancer. It is heartening to note that the efforts of government, media,hospitals, healthcare institutions, centres, and doctors all are geared towards educating public for early detection of the dreaded disease.
But unfortunately data tells us that today around 70% of cancer patients reach at stage 4 (incurable cancer) either at the time of diagnosis or even while taking the best possible treatment. We are not paying adequate attention to the lack of awareness and early screening that exists about cancer in the country.
Palliative care is what is required at this advanced stage. Pain management is the most important part of palliative care. Research has shown that palliative care & pain management provided by pain & palliative specialist is most effective in improving quality of life of the patient and mitigating the suffering of patients.
So, the most acute problem in these advanced-stage cancer patients is unbearable pain.With the help of modern medicines and advanced techniques,a majority ofthese patients can get adequate pain relief.
Problem
Big myth in the minds of patients – Cancer hai to dard to hoga hi. Advanced/Incurable cancer ho gaya to ab to dard mai rehna hi padega(If there is cancer, pain will inevitably happen. In the case of advanced/incurable cancer, one will have to live with pain).
Patients need to be made aware and educated.Though patients keep running for cancer cure treatment, they don’t expect pain relief as a goal in itself.Doctors, in general,do not focus on mitigating pain.
Pain management experts are not easily available. Probably Action Cancer Hospital (ACH) is the only hospital in private sector all over north India, which has a dedicated pain management department and experts. Specialized pain medicines are not easily available.
Pain Management Treatment
Specialized medicines like morphine, fentanyl, buprenorphine etc.
Advanced techniques known as MIPI (Minimally Invasive Pain Relief Intervention) These techniques stop the passage of pain by attacking pain sensation carrying nerves of cancer area or main passage nerves in spine with the help of needle like instruments & RF Ablation and some special medicines. And without any surgery or incision.
Latest technique of injection of medical cement for spine bone cancers not only controls pain and cancer but also prevent bones from fracture or collapse.
Revolutionary & state-of-the art pain relief implants, known as pacemaker of spine.
Pain Is Treatable At Any Or At Every Stage Of Cancer. Now Advanced Cancer Does’nt Mean Unavoidable Pain. We Can Offer A Pain-Free Journey For Cancer Patiemts.
(The author is Interventional Pain Management Specialistand Senior Consultant, Spine-Pain & Cancer Pain at Shri Balaji Action Medical Institute and Action Cancer Hospital, New Delhi)