Ayushman Bharat: High on promise, low on delivery
 Decades of neglect and a shift towards privatisation have left India’s healthcare system riddled with inequities. Despite efforts like Ayushman Bharat, corruption and inefficiency continue to plague public health initiatives, leaving millions without adequate care….
Decades of neglect and a shift towards privatisation have left India’s healthcare system riddled with inequities. Despite efforts like Ayushman Bharat, corruption and inefficiency continue to plague public health initiatives, leaving millions without adequate care….
Dr Amitav Banerjee
Private treatment does not always translate into quality care at an affordable cost. Competition is fierce in both business and medicine, which have become increasingly commercialised. In a single year in 2012, 55 million Indians were estimated to have fallen below the poverty line due to “catastrophic spending” on medical bills.
Our country’s improvement in health indicators, has not kept pace with our economic development. Although India was a signatory to the Alma Ata declaration of 1978, which pledged Health for All citizens of the world by the year 2000, its performance has been far from satisfactory. Key principles of delivery of healthcare are equitable distribution, community participation, inter-sectoral coordination, and appropriate technology, declared during the global “tryst on health,” at Alma Ata.
A vast country like India has multiple challenges in delivery of equitable healthcare. Besides the accessibility issue, the quality of healthcare is also an important dimension which poses an equal if not greater challenge. Our country is burdened by health inequalities as a consequence of many geo-social & political influences that aggravate healthcare further upon interacting with other determinants of health such as access to safe water, nutrition, housing, sanitation and education.
Health never attained the status of a right – the Inheritance of Loss
Public healthcare was neglected by the British rulers during their colonisation. This legacy of a weak foundation of a public health infrastructure adversely influenced the formulation of a robust health policy after independence. Detailed deliberations on health never took place in the Constituent Assembly debates between 1946 and 1950 by the founders of independent India. In the final draft of the Constitution, health is relegated to the Directive Principles, where it forms part of “the programme of social transformation …… to be realised in the fullness of time,” rather than being included in Article 21, which includes the right to life. The newly independent government also did not prioritise equitable public healthcare and further developments only widened the inequities in access to healthcare. The idea of public healthcare never attained political priority and surprisingly it has been consistently neglected even in times of high economic growth.
The Economic Liberalisation of the early 1990s and a paradigm shift favouring private players in providing healthcare.
The Indian economy underwent liberalised restructuring in the early 1990s. The impact on healthcare of this economic transition was catalytic. Tax exemptions, subsidised allotment of lands, and lower import tariffs on medical equipment encouraged private players to foray into healthcare. This was a turning point weaning the medical profession away from a calling to a business. In the decades following this paradigm shift, the private sector contributed to 70% of the increase in total hospital beds across the country.
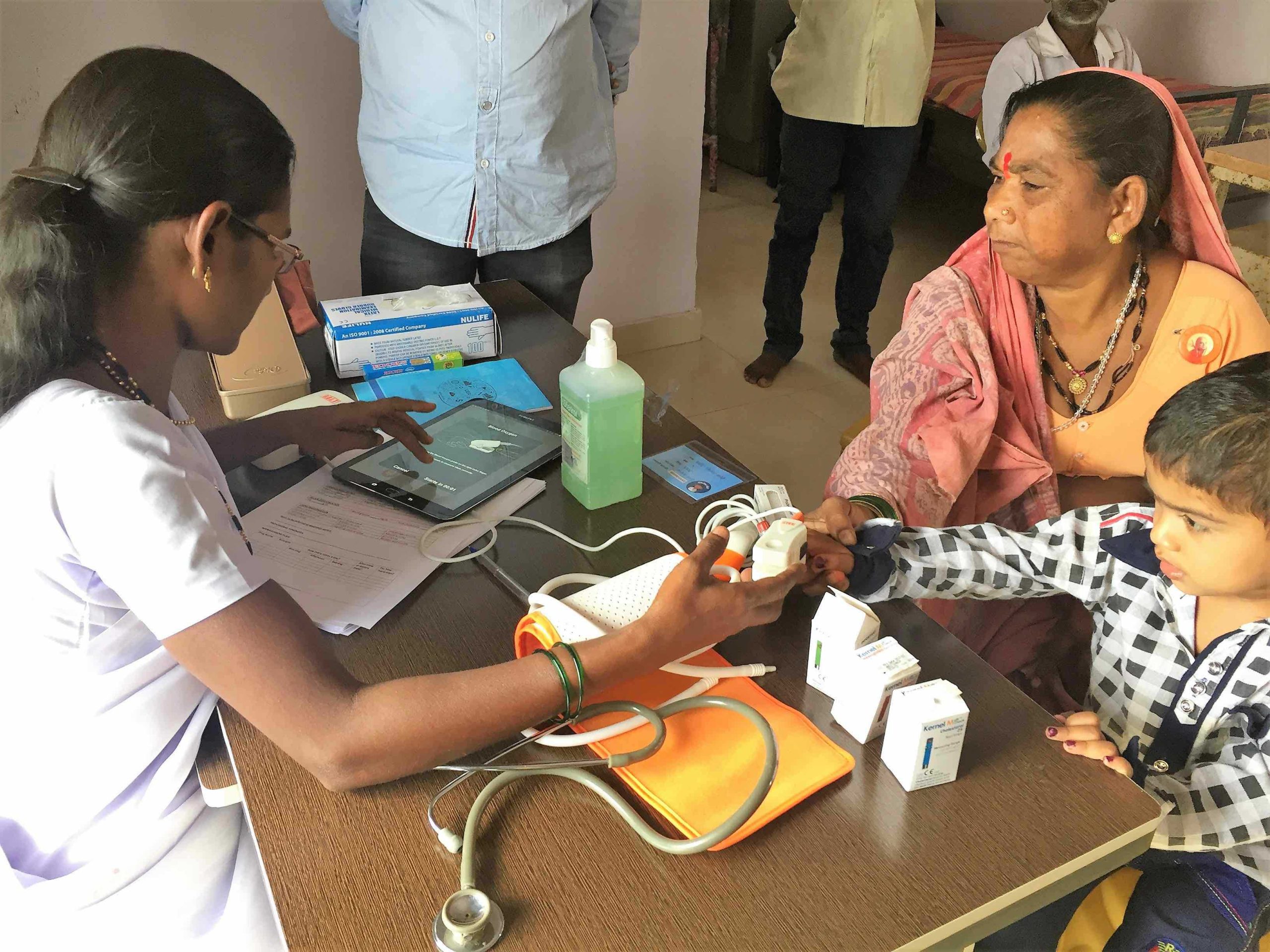
In cities, medical care may appear to be accessible, but it may be of dubious quality and can be financially devastating. On the other hand, increased allowance and private health insurance enabled some people to end their dependence on government health facilities, and flaunt their choice of high-end private hospitals as a “status symbol.”
But for the majority seeking private care it was a necessity rather than a status given the decay in our public health infrastructure as a consequence of decades of neglect. This resulted in increasing “out-of-pocket” expenditure and often “catastrophic spending” pushing many to below the poverty line.
Paradigm shift towards private players in healthcare further impoverished the public health sector.
India’s shortage of doctors is well known. What is more important is the unequal distribution both in terms of urban-rural differences and public-private sectors. Rural India where 70% of our population live is served by only 30% of the doctors. The contrast between the proportion of doctors serving in the public and private sector is starker. Around 11% of them work in the public sector out of which barely 3% are in rural areas. Given this skewed distribution which shows no sign of balancing, one can question whether producing more doctors would solve the country’s health problems.
Efforts made to improve the health of the people since Independence.
Our government has implemented many national programs from time to time since independence with mixed results. The National Rural Health Mission (NRHM), launched in 2005 addressed rural healthcare which was in a state of neglect for many years. The NRHM laid the foundation for the more ambitious National Health Mission (NHM), which has two components: the NRHM and the National Urban Health Mission. The thrust is on improving and strengthening infrastructure in both rural and urban areas. While these programs were well planned, their execution in our large country with its regional disparities posed many challenges.

National Health Policy 2017, Ayushman Bharat Program. A thin coat of paint on the underbelly of our poor health infrastructure and a thick coat on the surface.
With much promise and expectations, the bold and ambitious Ayushman Bharat Program (ABP) was included in the Union Budget of 2018-19. The ABP consisted of two strategies: first, the delivery of comprehensive primary level healthcare by upgrading 150,000 health subcentres (SC) and Primary Health Centres (PHC) to Health and Wellness Centres (HWC) by the year 2022, and secondly, catering for secondary and tertiary level medical care under Pradhan Mantri Jan Arogya Yojana (PMJAY). It was claimed that PMJAY is the world’s largest health program. What is paradoxical is that no significant financial provisions were made to beef up the ailing public health infrastructure in the country.
For example, the Finance Ministry allocated Rs 1,200 crore for the health and wellness centres in 2018-19 which translates to Rs 80,000 per centre. Essentially it was just a thin coat of paint for the old primary healthcare centres which were renamed for the occasion. The PMJAY got a slightly thicker coat of paint. The budget allocation for PMJAY at the launch in 2018-19 was Rs 2,000 crore, which was twice the previous year’s budget for the Rashtriya Swastha Bima Yoyana, the PMJAY’s predecessor, which got engulfed under the PMJAY. Essentially, both of the components of the Ayushman Bharat Program, the HWCs and the PMJAY were old wine in new bottles.
The goal of the PMJAY was to provide health insurance cover of Rs 5 lakhs to 10 crore families (around 50 crore beneficiaries). It was projected to be the world’s largest government funded healthcare program. This was not exactly correct. The scheme covered breadth but lacked in depth.
Many hospitals are empanelled without proper checks.
Around 30,000 hospitals are empanelled across the country for providing services under the scheme. All public hospitals with beds, from Community Health Centre Level and above are deemed empanelled. A little over 15,000 public and 12,000 private healthcare facilities are empanelled.

The empanelled hospital has to have minimum facilities such as pharmacy, blood bank, lab, dialysis, ICU and so on.
The CAG found deficiencies in these standards in some healthcare facilities, as well as instances of hospitals getting empanelled without proper checks.
As a result, many hospitals were unable to provide the promised services and the beneficiaries had to spend money to travel to bigger centres or resort to “out of pocket” expenditure that defeated the very purpose of the PMJAY.
Takeaways
There are no short cuts to population health. The foundation for this lies in strengthening of the less glamorous peripheral health centres and district hospitals. Special incentives and facilities are required to attract doctors and health auxiliaries to serve in the rural areas where the majority of our population lives. Privatisation and corporatisation of healthcare will thrive in the vacuum created by the lack of proper public health infrastructure.
If basic health facilities are not available to the vast majority of the rural population and if the beneficiaries have to spend on travel to cities to avail of the benefits under the scheme, then the very purpose of the ABP will be defeated. While they may save on out-of-pocket expenditure for medical treatment, they will spend many times more on travel and lodging and boarding for those accompanying the patient.
The CAG report is disturbing. It points at exploitation of the poor beneficiaries most likely through middlemen and touts. Medical insurance frauds are well known even in developed countries. For a vast country like India with poor checks and balances such schemes are not likely to achieve the goal of health for all. It is a sorry state of affairs, indeed.
(The author, a renowned epidemiologist, is currently a professor at a Medical College in Pune, India. Having served as an epidemiologist in the armed forces for over two decades, he recently ranked in Stanford University’s list of the world’s top 2% scientists.)

