Combating The Parasite
RTS, S, the world’s first malaria vaccine that has been shown to provide partial protection against malaria in young children, is being made available through routine immunization programmes, supported by WHO….
By Dr Suneela Garg/ Dr Samar Hossain


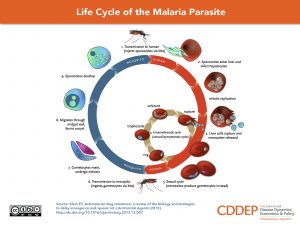
Malaria is a life-threatening mosquito-borne blood disease. The Anopheles mosquito transmits it to humans. The parasites in mosquitoes that spread malaria belong to the Plasmodium genus. Over 100 types of Plasmodium parasite can infect a variety of species. Different types replicate at different rates, changing how quickly the symptoms escalate, and the severity of the disease.
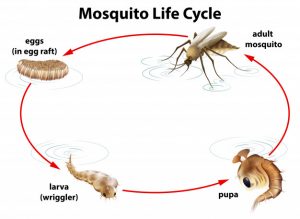 Mosquito transmission cycle
Mosquito transmission cycle
Uninfected mosquito – A mosquito becomes infected by feeding on a person who has malaria.
Transmission of parasite – If this mosquito bites you in the future, it can transmit malaria parasites to you. In the liver – Once the parasites enter your body, they travel to your liver — where some types can lie dormant for as long as a year.
Into the bloodstream – When the parasites mature, they leave the liver and infect your red blood cells. This is when people typically develop malaria symptoms.
On to the next person – If an uninfected mosquito bites you at this point in the cycle, it will become infected with your malaria parasites and can spread them to the other people it bites.
Other modes of transmission
Because the parasites that cause malaria affect red blood cells, people can also catch malaria from exposure to infected blood, including:
a)From mother to unborn child
b)Through blood transfusions
c)By sharing needles used to inject drugs
Risk factors-
The biggest risk factor for developing malaria is to live in or to visit areas where the disease is common. There are many different varieties of malaria parasites. The variety that causes the most serious complications is most commonly found in:
African countries south of the Sahara Desert
The Asian subcontinent
New Guinea, the Dominican Republic and Haiti
 Complications
Complications
In most cases, malaria deaths are related to one or more serious complications, including:
Cerebral malaria – If parasite-filled blood cells block small blood vessels to your brain (cerebral malaria), swelling of your brain or brain damage may occur. Cerebral malaria may cause seizures and coma.
Breathing problems – Accumulated fluid in your lungs (pulmonary edema) can make it difficult to breathe.
Organ failure – Malaria can cause your kidneys or liver to fail, or your spleen to rupture. Any of these conditions can be life-threatening.
Anemia – Malaria damages red blood cells, which can result in anemia.
Low blood sugar – Severe forms of malaria itself can cause low blood sugar (hypoglycemia), as can quinine — one of the most common medications used to combat malaria.
 The Vaccine-
The Vaccine-
The complexity of the malaria parasite makes development of a malaria vaccine a very difficult task. Recent progress has been made with the completion of a Phase 3 trial of the RTS, S/AS01 candidate vaccine and review by the European Medicines Agency and WHO. There is currently no commercially available malaria vaccine. Over 20 other vaccine constructs are currently being evaluated in clinical trials or are in advanced preclinical development.
RTS, S/AS01 is the most advanced vaccine candidate against the most deadly form of human malaria, Plasmodium falciparum. A Phase 3 trial with 15460 children in seven countries in sub-Saharan Africa (Burkina Faso, Gabon, Ghana, Kenya, Malawi, Mozambique, and the United Republic of Tanzania) began in May 2009 and has now been completed.
There were two age categories in the trial:
A) Children aged 5-17 months at first dose receiving the RTS, S/AS01 vaccine or a comparator vaccine; and
B) Children aged 6-14 weeks at first dose who receive the RTS, S/AS01 vaccine or a comparator vaccine in co-administration with the pentavalent vaccine from the routine immunization schedule.
All children received 3 doses of study vaccines vaccine at 1 month intervals. The role of a fourth dose 20 months after the first dose was also evaluated.
WHO Ghana welcomed the Ministry of Health’s launch of the world’s first malaria vaccine in a landmark pilot programme. Top health officials, WHO representatives, community leaders, and mothers and children gathered on 30 April 2019 to officially begin the vaccine rollout. The country-led phased vaccine introduction is supported by WHO, national and global health partners.
RTS, S/AS01 (RTS, S) is the world’s first malaria vaccine that has been shown to provide partial protection against malaria in young children. The vaccine acts against Plasmodium falciparum, the most deadly malaria parasite globally and the most prevalent in Africa.
Ghana is one of three African countries in which the vaccine, known as RTS, S, will be made available to children up to 2 years of age. Susana and Abigail, both age 6 months, were then vaccinated – the first children to receive the malaria vaccine in the Ghana pilot – in front of the attending audience of about 300 health workers, national immunization and malaria specialists and community supporters. RTS, S is the first, and to date the only, vaccine that has been found to significantly reduce malaria in children. In clinical trials, the vaccine was found to prevent approximately 4 in 10 malaria cases, including 3 in 10 cases of life-threatening severe malaria.
The vaccine will be made available through routine immunization programmes to young children living in selected areas in Ghana, Kenya and Malawi. Immunization authorities in the 3 countries will specify the vaccination schedule, based on WHO recommendations. A 4-dose schedule is required, with the first dose given as soon as possible after 5 months of age followed by doses 2 and 3 at approximately monthly intervals and the fourth dose near the child’s second birthday.
Important facts
1. The vaccine offers no protection against P. vivax malaria, which predominates in many countries outside of Africa.
2. These countries included: Burkina Faso, Gabon, Ghana, Kenya, Malawi, Mozambique, and the United Republic of Tanzania.
3. Severe malaria refers to those cases where the initial infection with the malaria parasite evolves into an acute, life-threatening illness.
4. Specifically, they will evaluate the feasibility of delivering the vaccine in real-life settings, the impact of the vaccine on childhood survival and the vaccine’s safety profile in the context of routine use.
5. In 2017, malaria killed an estimated 266000 under-fives globally.
(The authors are Director Professor HAG/Senior Resident, Department of Community Medicine, Maulana Azad Medical College, New Delhi)

