A Continental Crisis
 A landmark study spanning three decades reveals a dramatic surge in metabolic diseases across Asia. However, widespread adoption of balanced diets, regular physical activity, and proactive clinical surveillance can significantly reverse the tide
A landmark study spanning three decades reveals a dramatic surge in metabolic diseases across Asia. However, widespread adoption of balanced diets, regular physical activity, and proactive clinical surveillance can significantly reverse the tide
By Dr Anoop Misra
Alandmark study recently conducted by Zhang and colleagues, co-authored by the author, provides a sobering look at the health trajectory of the continent. Analysing data spanning from 1990 to 2023, the research demonstrates that the burden of metabolic diseases has increased exponentially over the past three decades in Asia. This upward trend shows no signs of slowing down; experts project that these figures will continue to rise through 2030. Currently, five major non-communicable diseases (NCDs) are driving this surge, fundamentally altering the public health landscape of the region and placing unprecedented pressure on healthcare infrastructure. uncertainties, even the manufacturers of the vaccines recommend that even after taking the HPV vaccine , women should keep undergoing periodic screening with PAP smear for early detection of cervical cancer.
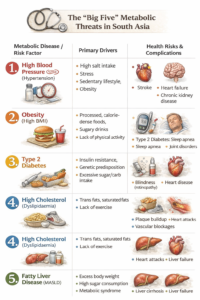
The Interconnected “Big Five” in South Asia
In South Asia, the crisis is defined by five specific metabolic diseases and risk factors that are increasing sharply. These include high blood pressure, obesity (high body mass index), high cholesterol, type 2 diabetes, and fatty liver disease. Among these, high blood pressure represents the most significant disease burden in the Asia–Pacific region, closely followed by obesity and abnormal cholesterol levels. Diabetes is also rising at an alarming rate, affecting millions of people in India and neighbouring countries. Of particular concern to clinicians is the fact that these conditions are appearing at much younger ages than in previous generations, leading to longer lifetimes of managed illness and higher risks of early complications.

Drivers of Metabolic Dysfunction
The roots of this modern epidemic are deeply embedded in the rapid urbanisation and socio-economic shifts occurring across Asian nations. As traditional lifestyles give way to modern conveniences, unhealthy diets—characterised by the high consumption of processed foods, sugary drinks, and high-fat meals—have become the norm. This nutritional transition is compounded by a significant reduction in physical activity, as more individuals spend prolonged periods sitting at desks or engaged with digital devices. These factors, combined with escalating stress levels, disrupt the body’s delicate hormonal balance. The result is a widespread increase in body weight and metabolic impairments that damage the heart, liver, kidneys, and blood vessels. These conditions are dangerous because they disrupt the body’s normal metabolism and increase the risk of several serious diseases that affect the heart, liver, kidneys, and blood vessels. Rapid urbanisation, unhealthy diets, reduced physical activity, and increasing stress levels are major reasons for this trend. As people consume more processed foods, sugary drinks, and high-fat diets while spending more time sitting at desks or using digital devices, body weight and metabolic problems are increasing.
 Metabolic diseases share common roots. As illustrated by a typical clinical case of advanced metabolic multimorbidity, their convergence often leads to catastrophic outcomes including heart attacks, strokes, kidney failure, and irreversible liver damage.
Metabolic diseases share common roots. As illustrated by a typical clinical case of advanced metabolic multimorbidity, their convergence often leads to catastrophic outcomes including heart attacks, strokes, kidney failure, and irreversible liver damage.
Bhavya Arora
A Cascade of Health Complications
These metabolic conditions do not exist in isolation; they are intricately linked in a dangerous physiological cycle. For instance, obesity significantly heightens the risk of developing diabetes, hypertension, and fatty liver disease simultaneously. When left unmanaged over time, this cluster of disorders leads to catastrophic health events, including heart attacks, strokes, kidney failure, and permanent liver damage. The ripple effect of these complications extends beyond the individual, placing an exhausting financial and emotional burden on families and creating a sustainability crisis for national health-care systems.
Case Illustration: The Reality of Metabolic Multimorbidity
A 56-year-old male presented with fatigue, increased urination, increased thirst, breathlessness on minimal exertion, and swelling of feet. He had a long-standing history of smoking (over 20 years), a sedentary lifestyle, and poor dietary compliance with high intake of refined carbohydrates and processed foods. On examination, his weight was 110 kg, corresponding to a body mass index (BMI) of 43 kg/m² (severe obesity). Blood pressure was elevated at 160/100 mmHg. His laboratory investigations revealed: fasting blood glucose: 210 mg/dL; HbA1c: 9.5% (poor glycaemic control); lipid profile: elevated triglycerides (blood fat) and low HDL cholesterol. The ultrasound abdomen showed enlarged liver with size of 19 cm, fibroscan (test to measure liver stiffness) demonstrated evidence of damage in liver. The patient was diagnosed with: poorly controlled type 2 diabetes, uncontrolled blood pressure (hypertension), severe obesity (BMI >40 kg/m²), high blood cholesterol (hypercholesterolemia), and fatty liver with marked stiffness [metabolic dysfunction-associated steatotic liver disease (MASLD) with fibrosis]. This case illustrates advanced metabolic multimorbidity, characterised by the coexistence of type 2 diabetes, hypertension, severe obesity, dyslipidaemia, and metabolic dysfunction-associated steatotic liver disease, all conditions which require major lifestyle and drug changes. These conditions share common pathophysiological mechanisms primarily insulin resistance, excess fat in abdomen, and chronic low-grade inflammation and typically cluster together, amplifying overall risk of heart disease and death in this context. In alignment with the findings of Zhang et al., 2026, the burden of these five metabolic diseases and risk factors has increased substantially across the Asia-Pacific region over the past three decades and is a measure of concern.
Despite the sobering statistics, health experts stress that the metabolic crisis is not inevitable. The cornerstone of prevention lies in sustainable lifestyle change: maintaining healthy weight through balanced, home-cooked meals rich in whole grains, pulses, fruits, and vegetables, while eliminating sugary drinks and processed snacks.
The Path to Prevention and Long-term Health
Despite the daunting statistics, there is a clear path forward through preventative lifestyle measures. Weight loss is essential for people who are obese. Maintaining a healthy body weight remains the cornerstone of metabolic health. People should eat a balanced diet that includes more fruits, vegetables, whole grains, pulses, and home-cooked foods while reducing fried foods, processed snacks, and sugary beverages. Regular physical activity such as brisk walking, cycling, yoga, or simple resistance exercises for at least 30–45 minutes most days of the week can help control weight, blood sugar, and blood pressure.
The Importance of Clinical Vigilance
Beyond diet and exercise, a holistic approach to health must include adequate sleep, effective stress management, and the avoidance of smoking and excessive alcohol consumption. Proactive medical surveillance is equally vital; regular health check-ups to monitor blood sugar, cholesterol, blood pressure, and body weight can help detect problems early and identify metabolic shifts before they become irreversible. By integrating these simple yet powerful habits into daily life, individuals and communities can effectively halt the progression of metabolic diseases and secure a healthier future for South Asia.
(The author is Chairman, Fortis-C-DOC Centre of Excellence for Diabetes, Metabolic Diseases and Endocrinology, New Delhi; Chairman, National Diabetes, Obesity and Cholesterol Foundation (N-DOC); and President, Diabetes Foundation (India) (DFI). Inputs provided by Bhavya Arora, A Clinical Nutritionist & Certified Diabetes)
Reference:
H. Zhang et al.; Burden of metabolic diseases, 1990-2023, with forecasts to 2030 for the Asia-Pacific region; Metabolism 179 (2026) 156575

